Breast cancer: The number one killer cancer in Somalia
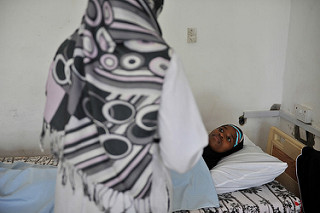
Worldwide, the month of October is set aside every year to promote breast cancer awareness and although general knowledge about this deadly disease is rising steadily, it provides little solace to communities with no health infrastructure.
In Somalia, data on breast cancer prevalence is anecdotal. The country’s fledgling health ministry has not documented cases of breast cancer, but the World Health Organization (WHO) statistics of May 2014 indicate that cancer kills at least 3,200 women in the country every year. Of these deaths, breast cancer is the single leading cause, accounting for 19-percent of the deaths, followed cervical cancer and cancer of the oesophagus.
Although cancer is mainly a genetic disease, a health practitioner based in Mogadishu Dr. Asha Omar Ahmed says it is difficult to trace the genetic risk in Somali families, because most of them never know what has killed a family member.
Against the odds
Breast cancer is a silent killer in many households in the horn of Africa country. Culturally, it is a disease treated in shame because it attacks the vital but extremely private parts of the female body. Most victims shy away from seeking medical help to avoid intrusion into their privacy.
“Traditionally Somali women are shy and there many things they cannot discuss with doctors. Even when they feel pain in their breasts, they shy away and keep the clothes on. If they are asked to explain, they cannot mention the word breast and would be unable to get treatment. They are shy to display breast swellings or wounds,” says Ms. Hamdi Abdullahi, a resident of Mogadishu who went through a breast cancer scare a few years ago.
In June 2012 while living in Hargeisa, the capital of the semi-autonomous Somaliland, Hamdi noticed a swelling on her breast, but took weeks to seek medical help. She was overwhelmed with worry for months until she gathered courage and visited the hospital. “It started like a boil on my breast. It became worse and caught an infection,” Hamdi relives her experience.
As she sought treatment for the infection, she moved to Mogadishu to be with her family, hoping to get some form of diagnosis from visiting Turkish doctors in the capital city. This did not happen. It is then that Hamdi sought help from the Somali National Women’s Organisation (SNWO), based in Mogadishu, who linked her with Blue Star Hospital, a private health facility that had been opened by a team of foreign doctors of Somali descent.
It is at this private hospital that Hamdi was finally screened for breast cancer by visiting oncologists from Kenya, in October 2013. For Hamdi, the heavens smiled down at her, because her swelling was found to be non-cancerous. “I had prepared myself for the after-life because I expected to die anytime. I had lost hope. After my tests, the doctors prescribed for me some medication for the breast infection which I couldn’t get in Somalia. I had to send for it from Germany. Thankfully Allah healed me,” says a beaming Hamdi.
Today, she is a protocol officer in the Office of the Deputy Prime Minister of Somalia.
For Hamdi, the state of helplessness she felt while seeking medication may have been short lived, but hundreds of other women in Somalia who find themselves in a similar situation are not as lucky, in a country where the health infrastructure
remains fragile, following more than two decades of war.
Cancer awareness levels
Somalia has one of the lowest levels of awareness for breast cancer, according to medical experts. This hinders early detection of the disease and compounds the process of management and cure. Somali culture that places sanctity on a woman’s body has also fuelled the spiral of silence about breast cancer, worsened by the fact that most oncologists in Somalia are male. “If the mother or sister has a lump, they will hide it. They don’t tell their husband. They don’t tell their brothers, or their sisters or their mothers. So what happens is that they keep the lump for some time until it becomes attached to the cloth and obviously starts to discharge,” says Dr. Mohamed Elmi, the proprietor of the Blue Star Hospital, one of the few private hospitals offering cancer screening services in Mogadishu.
The relative peace being enjoyed in the country has seen an aggressive attempt at the revival of the health infrastructure by the Federal Government and a robust participation by private health providers.
Female legislator in the Somalia Federal Parliament, Ms. Fowzia Mohamed Sheikh agrees that improving the country’s public healthcare system, would improve survival chances for women with breast cancer.
As a private health practitioner, Canadian-Somali Dr. Mohamed Elmi, returned home in 2012 and co-founded the Blue Star Hospital with other partners. The hospital provides public education on breast cancer, with free checkups and subsidized fees for mammogram and biopsies.
The facility partners with the Aga Khan Cancer Institute based in Nairobi, Kenya and also treats patients with chronic illnesses such as kidney ailments. “When it comes to cancer, we have seen around 40 patients in this hospital. We have many (types) of cancers including cancer of the tongue, esophagus, cancer of the colon, bladder,
prostate, breast and cancer of the brain. The commonest in women is breast cancer,” says Dr. Mohamed.
Due to low awareness levels and cultural considerations, most patients seek medical help when the cancer has advanced. To mitigate this, some hospitals have made deliberate efforts to hire female experts to help in handling female patients.
A female clinician working at the Blue Star Hospital Ms. Salome Ndeto explains, “We are coming up with ideas and that’s how as a clinician, I came in because the patients are more comfortable when I examine them since I am a female; compared to them being examined by a male doctor.”
Traditional Alternatives
Could traditional medicine provide an option in the management of cancers such as breast cancer? Dr. Mohamed disapproves of the traditional practice known as gubid, meaning to ‘treat’ breast cancer. The retrogressive practice, which is still practiced by some communities, involves burning a cancerous growth with red-hot iron, massaging the wound with hot water and taking herbs.
“They go to traditional doctors who start burning patients. If you have carcinoma of the tongue and there is a growth, they start burning the neck and the jaws. If you have breast cancer, they start burning the area of the tumor,” says Dr. Mohamed.
Dr. Asha recommends the introduction of mobile mammography in rural areas to expand screening services for women. This however, will require concerted efforts of all stakeholders in the health sector.